
Tobacco is a plant. Its leaves are smoked, chewed, or sniffed for a variety of effects.
- Tobacco is an addictive substance because it contains the chemical nicotine.
- Tobacco contains more than 19 known cancer-causing chemicals (most are called "tar.")
Health Risks Of Smoking Or Smokeless Tobacco
There are many more reasons to quit using tobacco. Knowing the serious health risks may help motivate you to quit. When used over a long period, tobacco and related chemicals such as tar and nicotine can increase your risk of many health problems.
- Heart and blood vessel problems:
- Blood clots and aneurysms in the brain, which can lead to stroke
- Blood clots in the legs, which may travel to the lungs
- Coronary artery disease, including angina and heart attacks
- High blood pressure
- Poor blood supply to the legs
- Problems with erections because of decreased blood flow into the penis
- Cancer (especially in the lung, mouth, larynx, esophagus, bladder, kidney, pancreas, and cervix)
- Poor wound healing, especially after surgery
- Lung problems such as emphysema and chronic bronchitis, or asthma that is harder to control
- Problems during pregnancy, such as babies born at low birth weight, premature labor, miscarriage, and cleft lip
Other health risks or problems:
- Decreased ability to taste and smell
- Harm to sperm, which contributes to infertility
- Loss of sight due to an increased risk of macular degeneration
- Tooth and gum diseases
- Wrinkling of the skin
Smokers who switch to smokeless tobacco instead of quitting tobacco completely still have a number of health risks:
- Increased risk of mouth or nasal cancer
- Gum problems, tooth wear, and cavities
- Worsening high blood pressure and angina
Health Risks Of Secondhand Smoke
Those who are regularly around the smoke of others (secondhand smoke) have a higher risk of:
- Heart attacks and heart disease
- Lung cancer
- Sudden and severe reactions, including those involving the eye, nose, throat, and lower respiratory tract
Infants and children who are regularly exposed to secondhand smoke are at risk of:
- Asthma (children with asthma who live with a smoker are much more likely to visit the emergency room)
- Infections, including virus-caused upper respiratory infections, ear infections, and pneumonia
- Lung damage (poor lung function)
- Sudden infant death syndrome (SIDS)
Don't give up!
Like any addiction, quitting tobacco is difficult, especially if you are acting alone. Most people who have quit smoking were unsuccessful at least once in the past. Try not to view past attempts to quit as failures. See them as learning experiences. It is hard to stop smoking or using smokeless tobacco. But anyone can do it.
Know the symptoms to expect when you stop. Common symptoms include:
- An intense craving for nicotine
- Anxiety, tension, restlessness, frustration, or impatience
- Difficulty concentrating
- Drowsiness or trouble sleeping
- Headaches
- Increased appetite and weight gain
- Irritability or depression
How bad your symptoms are depends on how long you smoked. How many cigarettes you smoked each day also plays a role.
Feel Ready To Quit?
First, set a quit date. Quit completely on that day. Before your quit date, you may begin reducing your cigarette use. But remember, there is no safe level of cigarette smoking.
List the reasons why you want to quit. Include both short- and long-term benefits.
Identify the times you are most likely to smoke. For example, do you tend to smoke when feeling stressed or down? When out at night with friends? While drinking coffee or alcohol? When bored? While driving? Right after a meal or sex? During a work break? While watching TV or playing cards? When you are with other smokers?
Let your friends, family, and co-workers know of your plan to stop smoking. Tell them your quit date. It can be helpful if they know what you are going through, especially when you are grumpy.
Get rid of all your cigarettes just before the quit date. Clean out anything that smells like smoke, such as clothes and furniture.
Make A Plan
Make a plan about what you will do instead of smoking at those times when you are most likely to smoke.
Be as specific as possible. For example, drink tea instead of coffee. Tea may not trigger the desire for a cigarette. Or, take a walk when you feel stressed.
Remove ashtrays and cigarettes from the car. Put pretzels or hard candies there instead. Pretend-smoke with a straw.
Find activities that focus your hands and mind. But make sure they are not taxing or fattening. Computer games, solitaire, knitting, sewing, and crossword puzzles may help.
If you normally smoke after eating, find other ways to end a meal. Play a tape or CD. Eat a piece of fruit. Get up and make a phone call. Take a walk (a good distraction that also burns calories).
Change Your Lifestyle
Make other changes in your lifestyle. Change your daily schedule and habits. Eat at different times, or eat several small meals instead of three large ones. Sit in a different chair or even a different room.
Satisfy your oral habits in other ways. Eat celery or another low-calorie snack. Chew sugarless gum. Suck on a cinnamon stick.
Go to public places and restaurants where smoking is prohibited or restricted.
Eat regular meals, and don't eat too much candy or sweet things.
Get more exercise. Take walks or ride a bike. Exercise helps relieve the urge to smoke.
Set Some Goals
Set short-term quitting goals and reward yourself when you meet them. Every day, put the money you normally spend on cigarettes in a jar. Later, buy something you like.
Try not to think about all the days ahead you will need to avoid smoking. Take it one day at a time.
Even one puff or one cigarette will make your desire for more cigarettes even stronger. However, it is normal to make mistakes. So even if you have one cigarette, you don't need to take the next one.
Available Treatments
Medications your health care provider prescribes can help you quit nicotine and tobacco and keep you from starting again. In general, nicotine replacement therapy benefits moderate-to-heavy smokers (people who smoke more than 15 cigarettes a day) the most. Here are some facts about using nicotine replacement therapy:
-By not cheating on the very first day of nicotine-replacement use, you can increase the chance of quitting permanently by tenfold.
-The more cigarettes you smoke, the higher the dose of nicotine replacement you may need at the start of therapy. Adding a counseling program will make you more likely to quit.
-Do not smoke while using nicotine replacement. It can cause nicotine to build up to toxic levels.
-Nicotine replacement helps prevent weight gain while you are using it. However, people are still at risk for gaining weight when they stop using all nicotine.
-The dose of nicotine should be slowly decreased.
Types Of Nicotine Replacement Therapy
Nicotine supplements come in several forms:
- Gum
- Inhalers
- Lozenges
- Nasal spray
- Skin patch
All of these work well if they are used correctly. People are more likely to use the gum and patches correctly than other forms of nicotine supplements.
Nicotine Patch
All nicotine patches are placed and used in similar ways:
- A single patch is worn each day and replaced after 24 hours.
- Place the patch on different areas above the waist and below the neck each day.
- Put the patch on a hairless spot.
- People who wear the patches for 24 hours will have fewer withdrawal symptoms.
- If wearing the patch at night causes odd dreams, try sleeping without the patch.
- People who smoke fewer than 10 cigarettes per day should start with a lower dose patch (for example, 14 mg).
Nicotine Gum or Lozenge
You can buy nicotine gum (Nicorette and others) or lozenges (Commit and others) without a prescription. Some people prefer lozenges to the patch, because they can control the nicotine dosage.
Tips for using the gum:
- If you are just starting to quit, chew 1 - 2 pieces each hour, but no more than 20 pieces a day.
- Chew the gum slowly until it develops a peppery taste. Then tuck it between the gum and cheek and store it there so that the nicotine can be absorbed.
- The goal is to stop using the gum by 6 months. Although using nicotine gum long-term is probably safer than smoking, research is needed to confirm this.
- Wait at least 15 minutes after drinking coffee, tea, soft drinks, and acidic beverages before chewing a piece of gum.
- People who smoke more than 25 cigarettes per day have better results with the 4 mg dose than with the 2 mg dose.
- Tobacco is an addictive substance because it contains the chemical nicotine.
- Tobacco contains more than 19 known cancer-causing chemicals (most are called "tar.")
Health Risks Of Smoking Or Smokeless Tobacco
There are many more reasons to quit using tobacco. Knowing the serious health risks may help motivate you to quit. When used over a long period, tobacco and related chemicals such as tar and nicotine can increase your risk of many health problems.
- Heart and blood vessel problems:
- Blood clots and aneurysms in the brain, which can lead to stroke
- Blood clots in the legs, which may travel to the lungs
- Coronary artery disease, including angina and heart attacks
- High blood pressure
- Poor blood supply to the legs
- Problems with erections because of decreased blood flow into the penis
- Cancer (especially in the lung, mouth, larynx, esophagus, bladder, kidney, pancreas, and cervix)
- Poor wound healing, especially after surgery
- Lung problems such as emphysema and chronic bronchitis, or asthma that is harder to control
- Problems during pregnancy, such as babies born at low birth weight, premature labor, miscarriage, and cleft lip
Other health risks or problems:
- Decreased ability to taste and smell
- Harm to sperm, which contributes to infertility
- Loss of sight due to an increased risk of macular degeneration
- Tooth and gum diseases
- Wrinkling of the skin
Smokers who switch to smokeless tobacco instead of quitting tobacco completely still have a number of health risks:
- Increased risk of mouth or nasal cancer
- Gum problems, tooth wear, and cavities
- Worsening high blood pressure and angina
Health Risks Of Secondhand Smoke
Those who are regularly around the smoke of others (secondhand smoke) have a higher risk of:
- Heart attacks and heart disease
- Lung cancer
- Sudden and severe reactions, including those involving the eye, nose, throat, and lower respiratory tract
Infants and children who are regularly exposed to secondhand smoke are at risk of:
- Asthma (children with asthma who live with a smoker are much more likely to visit the emergency room)
- Infections, including virus-caused upper respiratory infections, ear infections, and pneumonia
- Lung damage (poor lung function)
- Sudden infant death syndrome (SIDS)
Don't give up!
Like any addiction, quitting tobacco is difficult, especially if you are acting alone. Most people who have quit smoking were unsuccessful at least once in the past. Try not to view past attempts to quit as failures. See them as learning experiences. It is hard to stop smoking or using smokeless tobacco. But anyone can do it.
Know the symptoms to expect when you stop. Common symptoms include:
- An intense craving for nicotine
- Anxiety, tension, restlessness, frustration, or impatience
- Difficulty concentrating
- Drowsiness or trouble sleeping
- Headaches
- Increased appetite and weight gain
- Irritability or depression
How bad your symptoms are depends on how long you smoked. How many cigarettes you smoked each day also plays a role.
Feel Ready To Quit?
First, set a quit date. Quit completely on that day. Before your quit date, you may begin reducing your cigarette use. But remember, there is no safe level of cigarette smoking.
List the reasons why you want to quit. Include both short- and long-term benefits.
Identify the times you are most likely to smoke. For example, do you tend to smoke when feeling stressed or down? When out at night with friends? While drinking coffee or alcohol? When bored? While driving? Right after a meal or sex? During a work break? While watching TV or playing cards? When you are with other smokers?
Let your friends, family, and co-workers know of your plan to stop smoking. Tell them your quit date. It can be helpful if they know what you are going through, especially when you are grumpy.
Get rid of all your cigarettes just before the quit date. Clean out anything that smells like smoke, such as clothes and furniture.
Make A Plan
Make a plan about what you will do instead of smoking at those times when you are most likely to smoke.
Be as specific as possible. For example, drink tea instead of coffee. Tea may not trigger the desire for a cigarette. Or, take a walk when you feel stressed.
Remove ashtrays and cigarettes from the car. Put pretzels or hard candies there instead. Pretend-smoke with a straw.
Find activities that focus your hands and mind. But make sure they are not taxing or fattening. Computer games, solitaire, knitting, sewing, and crossword puzzles may help.
If you normally smoke after eating, find other ways to end a meal. Play a tape or CD. Eat a piece of fruit. Get up and make a phone call. Take a walk (a good distraction that also burns calories).
Change Your Lifestyle
Make other changes in your lifestyle. Change your daily schedule and habits. Eat at different times, or eat several small meals instead of three large ones. Sit in a different chair or even a different room.
Satisfy your oral habits in other ways. Eat celery or another low-calorie snack. Chew sugarless gum. Suck on a cinnamon stick.
Go to public places and restaurants where smoking is prohibited or restricted.
Eat regular meals, and don't eat too much candy or sweet things.
Get more exercise. Take walks or ride a bike. Exercise helps relieve the urge to smoke.
Set Some Goals
Set short-term quitting goals and reward yourself when you meet them. Every day, put the money you normally spend on cigarettes in a jar. Later, buy something you like.
Try not to think about all the days ahead you will need to avoid smoking. Take it one day at a time.
Even one puff or one cigarette will make your desire for more cigarettes even stronger. However, it is normal to make mistakes. So even if you have one cigarette, you don't need to take the next one.
Available Treatments
Medications your health care provider prescribes can help you quit nicotine and tobacco and keep you from starting again. In general, nicotine replacement therapy benefits moderate-to-heavy smokers (people who smoke more than 15 cigarettes a day) the most. Here are some facts about using nicotine replacement therapy:
-By not cheating on the very first day of nicotine-replacement use, you can increase the chance of quitting permanently by tenfold.
-The more cigarettes you smoke, the higher the dose of nicotine replacement you may need at the start of therapy. Adding a counseling program will make you more likely to quit.
-Do not smoke while using nicotine replacement. It can cause nicotine to build up to toxic levels.
-Nicotine replacement helps prevent weight gain while you are using it. However, people are still at risk for gaining weight when they stop using all nicotine.
-The dose of nicotine should be slowly decreased.
Types Of Nicotine Replacement Therapy
Nicotine supplements come in several forms:
- Gum
- Inhalers
- Lozenges
- Nasal spray
- Skin patch
All of these work well if they are used correctly. People are more likely to use the gum and patches correctly than other forms of nicotine supplements.
Nicotine Patch
All nicotine patches are placed and used in similar ways:
- A single patch is worn each day and replaced after 24 hours.
- Place the patch on different areas above the waist and below the neck each day.
- Put the patch on a hairless spot.
- People who wear the patches for 24 hours will have fewer withdrawal symptoms.
- If wearing the patch at night causes odd dreams, try sleeping without the patch.
- People who smoke fewer than 10 cigarettes per day should start with a lower dose patch (for example, 14 mg).
Nicotine Gum or Lozenge
You can buy nicotine gum (Nicorette and others) or lozenges (Commit and others) without a prescription. Some people prefer lozenges to the patch, because they can control the nicotine dosage.
Tips for using the gum:
- If you are just starting to quit, chew 1 - 2 pieces each hour, but no more than 20 pieces a day.
- Chew the gum slowly until it develops a peppery taste. Then tuck it between the gum and cheek and store it there so that the nicotine can be absorbed.
- The goal is to stop using the gum by 6 months. Although using nicotine gum long-term is probably safer than smoking, research is needed to confirm this.
- Wait at least 15 minutes after drinking coffee, tea, soft drinks, and acidic beverages before chewing a piece of gum.
- People who smoke more than 25 cigarettes per day have better results with the 4 mg dose than with the 2 mg dose.
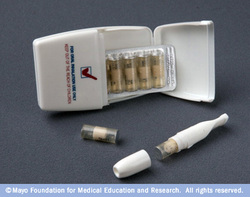
Nicotine Inhaler
The nicotine inhaler looks like a plastic cigarette holder. The nicotine inhaler requires a prescription in the United States.
- Insert nicotine cartridges into the inhaler and "puff" them for about 20 minutes, up to 16 times a day.
- The inhaler is fairly quick-acting, about the same as the gum and faster than the 2 - 4 hours it takes for the patch to work.
- The inhaler satisfies oral urges.
- Most of the nicotine vapor does not go into the airways of the lung. Some people notice mouth or throat irritation and cough.
- Using the inhaler and patch together can be very helpful when quitting.
Nicotine Nasal Spray
The nasal spray satisfies immediate cravings by providing quick doses of nicotine.
- It may be used along with the patch. Levels of nicotine peak within 5 - 10 minutes after using the spray.
- The spray can irritate the nose, eyes, and throat. These side effects often go away within the first few days.
Side Effects And Risks
Any of these nicotine products may cause side effects. Patients using very high doses are more likely to have symptoms. Reducing the dose can prevent these symptoms. Side effects include:
- Headaches
- Nausea and other digestive problems
- Problems getting to sleep in the first few days, most often with the patch. This problem usually passes.
Special Concerns
Nicotine patches pose no danger for people with heart or blood circulation problems. However, the unhealthy cholesterol levels (lower HDL levels) caused by smoking do not get better until the nicotine patch is stopped. Nicotine replacement may not be completely safe in pregnant women, although no real harmful effects have been reported. The unborn children of women who use the patch may have a faster heart rate. Keep all nicotine products away from children, especially small children. Nicotine is a poison.
- A parent should call a physician or a poison control center right away if a child has been exposed to a nicotine replacement product, even for a short time.
- Parents should watch for any symptoms, including stomach upset, irritability, headaches, a rash, or fatigue.
Smoking Cessation Medications
Bupropion (ZybanÂ)
Bupropion is a pill that may help decrease your craving for tobacco when you are trying to quit.
Although bupropion is also prescribed for people with depression, it will help with quitting tobacco, whether or not you have problems with depression. The exact way bupropion helps with tobacco cravings is not clear.
Bupropion is not FDA-approved for people under age 18, and is generally not used for those who:
- Are pregnant
- Have a history of seizures, kidney failure, heavy alcohol use, eating disorders such as anorexia or bulimia, bipolar or manic depressive illness, or a serious head injury
- How to take it:
- Bupropion works best if started 1 - 2 weeks before you stop smoking. You can take it for up to 6 months or a year.
- The most common dosage is 150 mg tablets once or twice per day.
- Taking bupropion along with nicotine patches, gums, or lozenges may work better for people who need help with cravings. Ask your doctor if this is okay for you.
Side effects that have been reported include:
- Dry mouth
- Problems sleeping. If this occurs, you can try taking the second dose in the afternoon, but it must be at least 8 hours after the first dose.
- Stop taking the medication right away if you have changes in behavior, hostility, agitation, depressed mood, suicidal thoughts and behavior, or attempted suicide.
The nicotine inhaler looks like a plastic cigarette holder. The nicotine inhaler requires a prescription in the United States.
- Insert nicotine cartridges into the inhaler and "puff" them for about 20 minutes, up to 16 times a day.
- The inhaler is fairly quick-acting, about the same as the gum and faster than the 2 - 4 hours it takes for the patch to work.
- The inhaler satisfies oral urges.
- Most of the nicotine vapor does not go into the airways of the lung. Some people notice mouth or throat irritation and cough.
- Using the inhaler and patch together can be very helpful when quitting.
Nicotine Nasal Spray
The nasal spray satisfies immediate cravings by providing quick doses of nicotine.
- It may be used along with the patch. Levels of nicotine peak within 5 - 10 minutes after using the spray.
- The spray can irritate the nose, eyes, and throat. These side effects often go away within the first few days.
Side Effects And Risks
Any of these nicotine products may cause side effects. Patients using very high doses are more likely to have symptoms. Reducing the dose can prevent these symptoms. Side effects include:
- Headaches
- Nausea and other digestive problems
- Problems getting to sleep in the first few days, most often with the patch. This problem usually passes.
Special Concerns
Nicotine patches pose no danger for people with heart or blood circulation problems. However, the unhealthy cholesterol levels (lower HDL levels) caused by smoking do not get better until the nicotine patch is stopped. Nicotine replacement may not be completely safe in pregnant women, although no real harmful effects have been reported. The unborn children of women who use the patch may have a faster heart rate. Keep all nicotine products away from children, especially small children. Nicotine is a poison.
- A parent should call a physician or a poison control center right away if a child has been exposed to a nicotine replacement product, even for a short time.
- Parents should watch for any symptoms, including stomach upset, irritability, headaches, a rash, or fatigue.
Smoking Cessation Medications
Bupropion (ZybanÂ)
Bupropion is a pill that may help decrease your craving for tobacco when you are trying to quit.
Although bupropion is also prescribed for people with depression, it will help with quitting tobacco, whether or not you have problems with depression. The exact way bupropion helps with tobacco cravings is not clear.
Bupropion is not FDA-approved for people under age 18, and is generally not used for those who:
- Are pregnant
- Have a history of seizures, kidney failure, heavy alcohol use, eating disorders such as anorexia or bulimia, bipolar or manic depressive illness, or a serious head injury
- How to take it:
- Bupropion works best if started 1 - 2 weeks before you stop smoking. You can take it for up to 6 months or a year.
- The most common dosage is 150 mg tablets once or twice per day.
- Taking bupropion along with nicotine patches, gums, or lozenges may work better for people who need help with cravings. Ask your doctor if this is okay for you.
Side effects that have been reported include:
- Dry mouth
- Problems sleeping. If this occurs, you can try taking the second dose in the afternoon, but it must be at least 8 hours after the first dose.
- Stop taking the medication right away if you have changes in behavior, hostility, agitation, depressed mood, suicidal thoughts and behavior, or attempted suicide.

Chantix Varenicline
Chantix helps with the craving for nicotine and withdrawal symptoms. It affects the brain, decreasing the physical effects of nicotine. So even if you start smoking again after quitting, you will not get as much pleasure from it.
How to take it:
- Your doctor will ask you to start taking this medication a week before you quit cigarettes. You will take it for 12 - 24 weeks.
- You should take it after meals with a full glass of water.
- Your doctor will give you instructions. Usually, you will be asked to take one 0.5 mg pill a day at first. By the end of the second week, you will likely be taking a 1 mg pill twice a day.
- Based on current research, this drug should not be combined with nicotine replacement therapy.
- Chantix is not FDA-approved, and therefore is not recommended for children under age 18.
Side effects are possible (although most of the time people tolerate varenicline well), including:
- NOTE: Use of this medication is associated with an increased risk of heart attack, stroke, and vascular problems.
- Headaches, problems sleeping, sleepiness, and unusual dreams
- Constipation, intestinal gas, nausea, and changes in taste
- Depressed mood, as well as thoughts of suicide and attempted suicide have been reported. Call your doctor right away if you have any of these symptoms.
Other Medicines
There is some evidence that the following medicines may be helpful in quitting smoking when the first-line medicines have not worked. However, their benefits are less consistent, and they are considered "second-line" treatment.
- Clonidine (Catapres), normally used to treat high blood pressure, increases the chance of smokers quitting when it is started before quitting in doses of 0.1 - 0.75 mg per day, either as a pill or patch.
- Nortriptyline, another antidepressant, increases the chance of smokers quitting when it is started 10 - 28 days before quitting in doses of 75 - 100 mg per day.
Programs Used in Conjunction with Medications
Like any addiction, quitting tobacco is difficult, especially if you are acting alone. Most smokers find it hard to break all the habits or ties they've built into their lives around smoking. By using smoking cessation programs, smokers may have a much better chance of success. Such programs are offered by hospitals, health departments, community centers, work sites, and national organizations. The best quit-smoking programs combine multiple strategies. All smoking cessation programs need to address and provide ongoing support for the many fears and difficulties you can encounter when quitting tobacco products.
Be wary of programs that:
- Are short and offer no help over time
- Charge a high fee
- Offer supplements or pills that are only available from the program
- Promise an easy path to quitting
Telephone-Based Help
Telephone counseling services are easy-to-use programs that can help you design a stop smoking program that works best for you. They can help you avoid making common mistakes.
Stop smoking telephone support can be a very helpful reinforcement, even as effective as face-to-face counseling.
Telephone programs are usually available nights and weekends. Trained counselors will help you decide whether you need medications, nicotine replacement therapy, and support programs or classes. They will help you set up a support network in your effort to quit cigarettes and tobacco.
A number of different telephone counseling smoking cessation programs are available or may be recommended by:
- Your local hospital or your physician
- Your health insurance plan
- Your employer
- The National Cancer Institute's 800-QUIT-NOW (800-784-8669)
- The American Cancer Society's Quitline at 800-ACS-2345 (800-227-2345)
- The American Lung Association, which has online and phone advice programs
- All 50 states and the District of Columbia run some type of free telephone-based program
Support Groups
Let all of your friends, family, and coworkers know of your plan to stop smoking and your quit date. Just being aware that they know what you're going through can be helpful - especially when you are grumpy.
However, you may want to seek out other types of support, such as:
- Your family doctor or nurse
- Groups of ex-smokers
- Nicotine Anonymous, an organization that uses a similar approach as Alcoholics Anonymous. As part of this group, you will be asked to admit that you are powerless over your addiction to nicotine. Also, a sponsor is often available over the long-term to talk when you have the temptation to smoke.
Check with your employer, health insurance plan, or health care provider about different types of support groups. Check the website of the American Cancer Society or American Lung Association for additional resources.
Stop Smoking Programs And Classes
Stop smoking programs also help you design an approach that works best for you. They will help you be more aware of problems that come up while you're trying to quit, and then give you tools to cope with these problems. They can help you avoid making common mistakes as you try to quit smoking.
Programs may either have one-on-one sessions or group counseling, or sometimes a combination of the two. Programs should be run by counselors who are trained in smoking cessation.
Programs that provide more counseling sessions or longer sessions have a better chance of success. The American Cancer Society recommends programs with the following:
- Each session lasts at least 15 - 30 minutes
- There are at least four sessions
- The program lasts at least 2 weeks -- longer is usually better
- The leader is trained in smoking cessation
Hospitals, employers, and health insurance plans all may provide this service. You can also call the local chapter of the American Cancer Society and the American Lung Association, or your local health department.
Increasingly, Internet-based programs are becoming available. They may send personalized reminders using e-mail, texting, or other methods.
The American Cancer Society's web site, www.cancer.org, is an excellent resource for smokers who are trying to quit. The Great American Smokeout can also help some smokers kick the habit.
Above all, don't get discouraged if you aren't able to quit smoking the first time. Nicotine addiction is a hard habit to break. Try something different next time. Develop new strategies, and try again. Many people take several attempts to finally kick the habit.
Chantix helps with the craving for nicotine and withdrawal symptoms. It affects the brain, decreasing the physical effects of nicotine. So even if you start smoking again after quitting, you will not get as much pleasure from it.
How to take it:
- Your doctor will ask you to start taking this medication a week before you quit cigarettes. You will take it for 12 - 24 weeks.
- You should take it after meals with a full glass of water.
- Your doctor will give you instructions. Usually, you will be asked to take one 0.5 mg pill a day at first. By the end of the second week, you will likely be taking a 1 mg pill twice a day.
- Based on current research, this drug should not be combined with nicotine replacement therapy.
- Chantix is not FDA-approved, and therefore is not recommended for children under age 18.
Side effects are possible (although most of the time people tolerate varenicline well), including:
- NOTE: Use of this medication is associated with an increased risk of heart attack, stroke, and vascular problems.
- Headaches, problems sleeping, sleepiness, and unusual dreams
- Constipation, intestinal gas, nausea, and changes in taste
- Depressed mood, as well as thoughts of suicide and attempted suicide have been reported. Call your doctor right away if you have any of these symptoms.
Other Medicines
There is some evidence that the following medicines may be helpful in quitting smoking when the first-line medicines have not worked. However, their benefits are less consistent, and they are considered "second-line" treatment.
- Clonidine (Catapres), normally used to treat high blood pressure, increases the chance of smokers quitting when it is started before quitting in doses of 0.1 - 0.75 mg per day, either as a pill or patch.
- Nortriptyline, another antidepressant, increases the chance of smokers quitting when it is started 10 - 28 days before quitting in doses of 75 - 100 mg per day.
Programs Used in Conjunction with Medications
Like any addiction, quitting tobacco is difficult, especially if you are acting alone. Most smokers find it hard to break all the habits or ties they've built into their lives around smoking. By using smoking cessation programs, smokers may have a much better chance of success. Such programs are offered by hospitals, health departments, community centers, work sites, and national organizations. The best quit-smoking programs combine multiple strategies. All smoking cessation programs need to address and provide ongoing support for the many fears and difficulties you can encounter when quitting tobacco products.
Be wary of programs that:
- Are short and offer no help over time
- Charge a high fee
- Offer supplements or pills that are only available from the program
- Promise an easy path to quitting
Telephone-Based Help
Telephone counseling services are easy-to-use programs that can help you design a stop smoking program that works best for you. They can help you avoid making common mistakes.
Stop smoking telephone support can be a very helpful reinforcement, even as effective as face-to-face counseling.
Telephone programs are usually available nights and weekends. Trained counselors will help you decide whether you need medications, nicotine replacement therapy, and support programs or classes. They will help you set up a support network in your effort to quit cigarettes and tobacco.
A number of different telephone counseling smoking cessation programs are available or may be recommended by:
- Your local hospital or your physician
- Your health insurance plan
- Your employer
- The National Cancer Institute's 800-QUIT-NOW (800-784-8669)
- The American Cancer Society's Quitline at 800-ACS-2345 (800-227-2345)
- The American Lung Association, which has online and phone advice programs
- All 50 states and the District of Columbia run some type of free telephone-based program
Support Groups
Let all of your friends, family, and coworkers know of your plan to stop smoking and your quit date. Just being aware that they know what you're going through can be helpful - especially when you are grumpy.
However, you may want to seek out other types of support, such as:
- Your family doctor or nurse
- Groups of ex-smokers
- Nicotine Anonymous, an organization that uses a similar approach as Alcoholics Anonymous. As part of this group, you will be asked to admit that you are powerless over your addiction to nicotine. Also, a sponsor is often available over the long-term to talk when you have the temptation to smoke.
Check with your employer, health insurance plan, or health care provider about different types of support groups. Check the website of the American Cancer Society or American Lung Association for additional resources.
Stop Smoking Programs And Classes
Stop smoking programs also help you design an approach that works best for you. They will help you be more aware of problems that come up while you're trying to quit, and then give you tools to cope with these problems. They can help you avoid making common mistakes as you try to quit smoking.
Programs may either have one-on-one sessions or group counseling, or sometimes a combination of the two. Programs should be run by counselors who are trained in smoking cessation.
Programs that provide more counseling sessions or longer sessions have a better chance of success. The American Cancer Society recommends programs with the following:
- Each session lasts at least 15 - 30 minutes
- There are at least four sessions
- The program lasts at least 2 weeks -- longer is usually better
- The leader is trained in smoking cessation
Hospitals, employers, and health insurance plans all may provide this service. You can also call the local chapter of the American Cancer Society and the American Lung Association, or your local health department.
Increasingly, Internet-based programs are becoming available. They may send personalized reminders using e-mail, texting, or other methods.
The American Cancer Society's web site, www.cancer.org, is an excellent resource for smokers who are trying to quit. The Great American Smokeout can also help some smokers kick the habit.
Above all, don't get discouraged if you aren't able to quit smoking the first time. Nicotine addiction is a hard habit to break. Try something different next time. Develop new strategies, and try again. Many people take several attempts to finally kick the habit.
 RSS Feed
RSS Feed
